Senate Inquiry into current barriers to patient access to medicinal cannabis in Australia.
January 2020
Cannabis Awareness Tasmania
Lyn Cleaver
Introduction.
In 2014 we began cannabis therapy for our adult son, Jeremy. Jeremy is diagnosed with severe refractory epilepsy and a ‘diffuse’ brain injury resulting from either Suspected Acute Viral Encephalitis or F.I.R.E.S (Febrile Infection-Related Epilepsy) which he contracted at age six in 1998.
Jeremy’s seizure diagnosis is partial onset seizures with secondary generalised tonic clonic seizures.

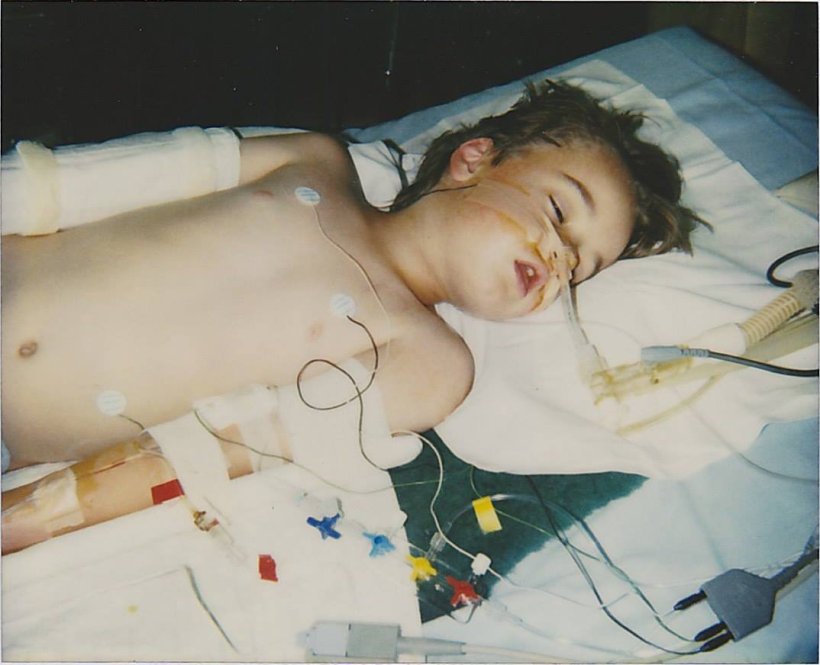
Jeremy is twenty eight years old.
At the time we commenced cannabis Jeremy was suffering from a serious drug induced psychosis from a prescribed anticonvulsant (AED). His treating neurologist informed us at that time he should try strong sedatives. To be clear, this measure was not for seizure control, rather for side effect control. At that time, his neurologist said he had nothing else suitable to prescribe for Jeremy to control his seizures.
Jeremy is not a brain surgery candidate as he has too many seizure foci across his brain. Jeremy was implanted with the Vagal Nerve Stimulator

at age eleven in an attempt to control his seizures. The device was not successful and while still in situ the generator is switched off due to side effects of uncontrolled coughing when the device malfunctioned during a lead impedance test.
Jeremy is recognised as being at very high risk of SUDEP (sudden unexplained death in epilepsy)
We started researching cannabis after discovering the health benefits of hemp seeds (which at that time; still illegal to consume) We were hopeful that cannabis would help with seizure control, the severe insomnia (directly caused by long term use of one particular AED) the toxicity he was suffering (caused by a drug interaction between two of the three AED’s he was taking at the time) and the explosive behaviours linked to the psychosis.
Jeremy was enduring weeks on end with little to no sleep. The toxicity was occurring almost daily where he would be ataxic, vomiting, nauseous and enduring blurred vision approximately fifteen minutes after being given his AED doses twice a day and lasting around an hour.
The psychosis, naturally, was the hardest for Jeremy and those of us around him to deal with. He was a danger to himself and to everyone around him. He hospitalised one of his support workers who was injured during a behaviour. Our daily lives were ruled by explosive behaviours, we locked all the doors and windows, put away objects that could be used as weapons, and basically lived by how he was feeling minute by minute. He was regularly trying to exit moving vehicles.
This was the second time Jeremy had experienced such a devastating psychosis, the first time occurring in his very early teenage years.
However, he was no stranger to unwanted or serious side effects from conventional AEDs below is a brief list of what Jeremy has endured from prescribed medicines;
Gum disease
Allergic reaction (medicine ceased immediately)
Weight gain
Weight loss
Refusal to eat
Relaxed throat muscles (added risk for aspiration)
Chronic insomnia
Cognitive delays
Toxicity
Inability to sweat
Increased seizures
Compromised respiratory function
Up until 2014 there was only one medicine that his paediatric neurologist wanted to prescribe that we were not willing for Jeremy to risk the serious side effect of this drug causing blindness.
When the neurologist suggested strong sedative drugs we knew that it was time to at least try cannabis as a chemical straight jacket is no life for anyone.
We were gifted some cannabis tincture and we commenced that in mid 2014.
It was evident almost immediately that cannabis was helping Jeremy in all the areas we hoped that it would. His sleeping patterns improved, his behaviours improved and his seizures were far less intense.
We then went on to purchase a supply (domestic) online. Evidenced by how well he was and the efficacy of the cannabis we started reducing his AED. We kept both his neurologist and his GP (Jeremy has been his patient for twenty five years) informed by alerting them to the fact we had started cannabis. Jeremy’s GP was extremely supportive and was encouraged by the benefits of using cannabis for Jeremy. He charted the cannabis medicines and helped advise us in the weaning process of the AED’s. His words at the time “They’ve never worked nor helped let’s try and wean them”
We purchased cannabis online for some months until suddenly one day we were told that “There was no medicine, supply is ceased”
We were horrified, cannabis had become essential in his medicine regime as we weaned the AED’s.
We were gifted some medicine from two dear friends, until we could work out what to do.
There seemed little choice – he couldn’t go back to the AEDs that were so ineffective and toxic to him, there was no other suitable AED’s for the neurologist to prescribe.

We started cultivating Jeremy’s medicine ourselves.

We have been open and upfront with Jeremy’s doctors, our then Premier Will Hodgman (at the time of writing we have no Premier), then Minister for Police Rene Hidding and then Minister for Health Michael Ferguson. We also contacted Tasmania Police.
Prior to the Controlled Access Scheme rolling out in September 2017, our leaders seemed to think that “You should be fine, Tasmania Police are not seeking out those who use medicinal cannabis”
Since then, and our failed attempt for Jeremy to be prescribed a cannabinoid medicine we are now being told by our leaders to “Choose a different medicine, and your use of illicit cannabis may compromise his future specialist care”
Our applications (since July 2017) for Jeremy have been met by a panel of experts the Tasmanian Medicines Access and Advisory Committee deciding that Jeremy must try and fail ALL conventional medicines before being eligible. We have also had to deal with his specialist ceasing care mid application process, and waiting for another neurologist to begin work at the hospital.
We were thankful to be assisted by a senior clinician at the Launceston General Hospital whose last correspondence to us was “You get the neurologist to apply and I will smooth the political waters”
At writing of this submission we are yet to decide if we will make another application for Jeremy to the Controlled Access Scheme.
The only thing we are certain of is that we will not expose Jeremy to medicines that were not ever deemed suitable for his neurologist to prescribe, that come with very serious side effects and according to his neurologist highly unlikely to control his refractory epilepsy.
While the risk to cultivate cannabis exposes us to having his medicine confiscated, being charged and limiting his independence out in the community we refuse to torture him with medicines that are ineffective and unsafe.
Cannabis is safe and effective for Jeremy and we will continue to offer him the best quality of life possible. After all he has endured and survived he deserves that much!
the appropriateness of the current regulatory regime through the Therapeutic Goods Administration (TGA) Special Access Scheme (SAS), Authorised Prescriber Scheme and clinical trials;
The current model should only considered appropriate when measured against patient experience.
For us and many Tasmanians the system is failing at the most basic levels. Access to specialists in Tasmania is extremely limited, lengthy wait lists of twelve months or more are common. Patients are being advised that certain out-patient clinics do “not provide that service” when patients seek a cannabinoid prescription.
We are acutely aware that even if there is a treating specialist willing to prescribe, and in some instances TGA approval already gained, the final say falls upon TMAAC.
(b) the suitability of the Pharmaceutical Benefits Scheme for subsidising patient access to medicinal cannabis products;
With limited understanding of this process it is understood that for a medicine to be approved, and then potentially listed on the PBS is a very lengthy process.
Of course, subsidised cannabis and medicinal cannabis products would benefit patients who cannot afford it now with the current pricing.
In Tasmania the medicines are subsidised and with only around a dozen patients approved this could hardly be called a success.
(c) the interaction between state and territory authorities and the Commonwealth, including overlap and variation between state and territory schemes;
Tasmania has not signed up to streamline access to cannabis and medicinal cannabis products.
Our understanding from Jeremy’s neurologist is that he was actually requested to CHANGE his initial prescription to a cheaper product. It is perhaps worth noting here that in comparison to the $60-100 thousand annual price tag for a legal prescription for Jeremy it costs us as little as $20 per week to provide him with home grown organic cannabis and cannabis medicines.
(d) Australia’s regulatory regime in comparison to international best practice models for medicinal cannabis regulation and patient access;
There is no doubt Australia has restricted cannabis and cannabis product access to the point where the current model actually drives patients to the alternative market and self supply.
If the current model was in place to protect patients self evidently it has been an abject failure.
(e) the availability of training for doctors in the current TGA regulatory regime for prescribing medicinal cannabis to their patients;
It does speak volumes that the patient often has more experience and knowledge of cannabis and medicinal cannabis products than their doctor.
Doctors and the other medical professionals need to be trained in the Endogenous Cannabinoid System (ECS). Their lack of knowledge should not be hindering patient access. Cannabis, compared to most medicine is very safe but doctors should be aware and educated in interactions with other prescribed medicines.
As if to signal a complete lack of understanding the TGA has developed clinical guidance documents for a very limited list of medical conditions. For example, guidelines exist for paediatric epilepsy but according to the guidelines there is no evidence to support prescribing to those epilepsy patients over the age of twenty five. Surely the authors understand children with epilepsy more often than not grow up to be adults with epilepsy?
(j) the impacts on the mental and physical wellbeing of those patients struggling to access medicinal cannabis through Australia’s regulatory regime;
When we first learnt about cannabis and went public with our fight for Jeremy we not long after this started Cannabis Awareness Tasmania. It is nothing more than an online social media presence. Tasmania is a small place with Cannabis Awareness Tasmania and the local media coverage fellow Tasmanians quickly learned of us, and what we were fighting for.
For this t.0.r I’d like to focus on these fellow Tasmanians, those who have contacted us in any number of ways over the years.
These Tasmanian patients matter and many of them wouldn’t even be aware of this current inquiry.
Keeping in mind I am not a doctor, pharmacist, social worker, psychologist or what some would consider a ‘professional advocate’ I have no other qualifications than mum and gardener – I’ll do my best to speak for them here;
In many ways the most difficult aspect of what we do is carrying the overwhelming experience of those who come to us for help or advice.
Sometimes when you receive online contact it is difficult to determine who is legitimate and who is not.
But then you just come across the most beautiful, desperately ill people that will do anything for help.
I’d like to make special mention of some of our fellow Tasmanians who have been spectacularly failed by our Government and the current system.
The many people suffering unimaginable chronic pain.
The young children with severely medication resistant epilepsy.
The mums and dads with uncontrolled epilepsy.
The young mum with stage four terminal cancer dumped by her doctor because she was beyond help.
Young Tasmanian patients trying to live well with epilepsy, fibromyalgia, cancer, endometriosis, and arthritis.
The Crohn’s sufferers.
The MS sufferers.
The chronic migraine sufferers.
The people with a myriad of mental health conditions.
The doctors who have somehow managed to get our personal numbers to have their patients call us.
The politicians who send their family, friends and constituents to us.
The complete strangers who come up our driveway. Who knock on our door and shake our hands and then burst into tears begging for help for their suffering and dying loved ones.
These Tasmanians deserve help, they need to be given a voice.
They deserve a doctor that listens, they deserve a panel at the end of that application that appreciates their lived experience and their desire to have a legal cannabis prescription.
They deserve a health minister who listens and is present.
They deserve a police minister who listens and is present.
They deserve a premier, a leader to actually stand up to fight for some of the most vulnerable people who are sick and dying in our state.
IN CONCLUSION
It hasn’t gone unnoticed that patients across Australia are yet again being asked to submit their experience. To this date, any legislation, regulation or policy has overwhelmingly not worked on behalf of the patient.
We call on the Government to appreciate and support the great number of patients who are self supplying their cannabis and medicinal cannabis products.
Of course, we are aware that many Australians do not want to grow their own medicine, and a great number can not self supply.
There is a relatively small number of Australians able to afford cannabis and cannabis products under the current scheme but that is completely overshadowed by the multitudes accessing the alternative market or those who are self supplying.
There is room for a tiered model –
Pharmaceutical grade cannabis and cannabis products.
Herbalist/Dispensary
Self supply.
In order for that to happen, cannabis and medicinal cannabis products must be rescheduled.
The current system is failing patients. Thousands of us are doing what we need to do – because we cannot afford the legal option, or because we cannot access a legal prescription.



